
Good day, dear readers!
In today's article we will look at diseases of the spine such as osteochondrosis, as well as its symptoms, causes, types, diagnosis, treatment and prevention.So...
What is osteochondrosis?
Osteochondrosis– diseases of the spine, the characteristic feature of which is degenerative-dystrophic damage to the intervertebral disc, and then to the vertebral tissue itself.
The main symptom of osteochondrosis is pain in the neck or back.Other symptoms include muscle atrophy, sensory disturbances, and disturbances in internal organ function.Depending on the location of the pathological process, they distinguish between cervical, thoracic and lumbar osteochondrosis.If this disease and its treatment are not given proper attention, the process of damage to the spine will become irreversible.
In English literature, the term "osteochondrosis" refers to a group of diseases of the musculoskeletal system such as osteochondropathy.
The main factor or reason that leads to the development of osteochondrosis is the uneven distribution of the load on the spine, which occurs when carrying a heavy object in one hand or shoulder (for example, a bag, a backpack), sitting for a long time in an incorrect position, resting at night on an uneven mattress or pillow.Additional factors may also include a sedentary lifestyle, obesity, injuries and flat feet.
All of the above situations lead to frequent pain in the cervical, thoracic or sacral spine for years.
According to statistics, osteochondrosis occurs in 40 to 90% of the world's population, especially between the ages of 30-35 years.Under unfavorable conditions, this disease develops in teenagers, which is most often facilitated by wearing a heavy and uncomfortable backpack, especially on one shoulder, uncomfortable shoes and injuries.
Development of osteochondrosis
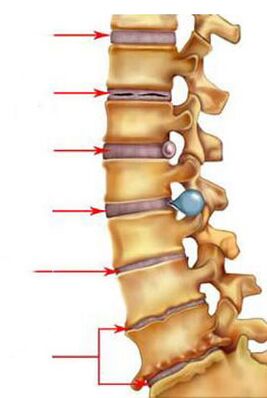
The development of osteochondrosis occurs in 4 stages (degrees):
Osteochondrosis stage 1.It is characterized by the beginning of the pathological process in the nucleus pulposus of the intervertebral disc - dehydration (dehydration) occurs, and subsequently the height of the disc decreases.At the same time, cracks begin to appear in the fibrous ring.At this stage, the patient usually does not feel any changes.Discomfort may occur when sitting in an unusual sitting position for a person, or when actively exercising.
Osteochondrosis stage 2.As the height of the disc decreases, the distance between adjacent vertebrae also decreases, and the muscles and ligaments of the spine begin to relax slightly.This process causes hypermobility of two adjacent vertebrae, which can cause them to slip and/or shift.Spondylolisthesis is formed.Due to the transferred vertebra, the patient, under a certain load, feels real discomfort and sometimes pain in the pathological area.
Osteochondrosis stage 3.It is characterized by the formation of prolapse and disc protrusion, sometimes subluxations and arthrosis occur in the intervertebral joints.Patients may feel stiffness in some movements, tingling in the limbs, and sometimes numbness appears.With osteochondrosis of the 3rd degree, there is already pain in the back, neck, and tailbone area, depending on the location of the disease.
Osteochondrosis stage 4.The body tries to correct excessive vertebral mobility, as well as normalize the function of the spine.At the junction of the vertebrae with pathology, new bone formations grow on each of them - osteophytes, which, when formed in an unnecessary place, can cause microtrauma to the nerve roots, and sometimes to neighboring vertebrae.Fibrous ankylosis may begin in the discs and joints.The vertebral-motor segment becomes too large and becomes, as it were, walled.In this case, the main signs of osteochondrosis are minimized, and sometimes almost imperceptible.
Symptoms of osteochondrosis
The main symptoms of osteochondrosis are discomfort and pain in the back or neck.The severity of pain and other symptoms that accompany this disease depends on the level (stage) of osteochondrosis.
Of course, due to the pathology of the intervertebral discs, their herniation, growths on the vertebrae (osteophytes), a large number of disorders occur, such as circulatory disorders, pinched nerves, irritation and disturbances in the normal function of the spinal cord, swelling and also structural fibrosis around the vertebrae.All these disorders can cause a wide clinical picture of the disease and are expressed by a large number of different symptoms, therefore, without a comprehensive diagnosis of osteochondrosis, it is very difficult to make a correct diagnosis and prescribe adequate treatment.
However, let's consider the main symptoms of osteochondrosis:
- pain in the back, cervical region, lower back, shoulders and even ribs;
- discomfort, back stiffness during certain movements, lifting something;
- numbness in the legs (arms and/or legs);
- pain in the arms and legs, shivering;
- muscle spasms;
- disorders in the function of the genital organs;
- headache, dizziness;
- pain in the heart area;
- sensory disturbances;
- muscle hypotension;
- increased fatigue, sometimes even in the eyes.
In addition, depending on the region of the spine affected by osteochondrosis, the following symptoms are distinguished:
Osteochondrosis of the cervical spine.Pain in the arms and shoulders, headaches, dizziness, spots or spots in front of the eyes, and noises in the head dominate.These signs may also indicate the presence of vertebral artery syndrome, which can also cause complications in the function of the heart muscle and myocardial vessels if other diseases are present in it.
Osteochondrosis of the thoracic spine.Pain in the chest, heart area and breathing discomfort are more dominant.
Osteochondrosis of the lumbosacral spine.Lower back pain predominates, radiating to the legs or pelvic organs.Sexual dysfunction.
Complications of osteochondrosis
If osteochondrosis is not treated and left to chance, it can lead to the development of the following diseases and pathologies:
- intervertebral disc herniation (spinal hernia);
- protrusion;
- kyphosis;
- radiculitis;
- salt deposition in the intervertebral space;
- spinal cord stroke;
- weight loss of limbs and their atrophy;
- paralyzed legs
Causes of osteochondrosis

The causes of osteochondrosis are not fully understood, so let's consider the most popular:
- mechanical injury to the back (spine);
- physical overstrain of the body, hard work;
- nervous exhaustion, stress;
- metabolic disorders, poisoning;
- often stay in places with increased vibration;
- hereditary predisposition;
- sedentary lifestyle, sedentary work;
- poor posture at an early age;
- overweight, obesity;
- flat feet;
- wearing uncomfortable shoes (tight, heels);
- night rest on an uncomfortable bed - mattress, pillow;
- frequent dehydration;
- malnutrition, hypovitaminosis;
- smoking;
- pregnancy.
Classification of osteochondrosis
The classification of osteochondrosis is very diverse, because the disease itself is not fully understood.
Let us highlight the most popular method of dividing this disease.
I distinguish osteochondrosis:
By localization:
- Cervical area ©
- Thorax (Th or D)
- Lumbar (L)
- sacral area (S)
According to clinical manifestations:
1. Cervical level ©.
1.1.Reflex syndrome.
- cervicgia;
- cervicocranialgia;
- cervicobrachialgia with vegetative-vascular, neurodystrophic or muscle-tonal manifestations.
1.2.Radicular syndrome.
- Discogenic lesions at the root of the cervical spine.
1.3.Radicular-vascular syndrome.
2. Thoracic level (Th or D).
2.1.Reflex syndrome.
- thoracalgia with vegetative-visceral, neurodystrophic or muscle-tonal manifestations.
2.2.Radicular syndrome.
- Discogenic lesions at the root of the thorax.
3. Lumbosacral level (L, S).
3.1.Reflex syndrome.
- lumbago (lumbago);
- lumbodynia;
- lumboischialgia with vegetative-vascular, neurodystrophic or muscle-tonal manifestations.
3.2.Radicular syndrome.
- Discogenic damage to the roots of the lumbosacral region.
3.3.Radicular vascular syndrome - radiculoischemia.
Diagnosis of osteochondrosis
Diagnosis of osteochondrosis includes the following examination methods:
- anamnesis;
- X-ray examination (X-ray);
- myelography;
- neurological examination.
In addition, they can set:
- computed tomography (CT);
- nuclear magnetic resonance (NMR);
- magnetic resonance imaging (MRI).
Treatment of osteochondrosis

The treatment of osteochondrosis involves the use of a set of measures that must be carried out over a relatively long period of time (from 1-3 months + about 1 year for recovery), to which many patients respond very ambiguously.Therefore, it should be noted that, by indirectly following the recommendations of the attending physician, the prognosis for the patient's recovery is minimal.
Medications themselves are often an additional problem in the treatment of osteochondrosis.The fact is, as it was written earlier in the article, with this disease the clinical picture is rather vague and broad.The patient, without a diagnosis, begins to choose medicine for what hurts, and, eliminating the pain, continues to live his daily life, while the disease continues to develop.
Important!Timely consultation with a doctor, a comprehensive health diagnosis and strict adherence to all the recommendations of the attending physician increase the positive prognosis for recovery!
Treatment of osteochondrosis is carried out by two main methods: conservative treatment and surgery.In addition, there are general recommendations for the treatment of osteochondrosis, such as diet and rehabilitation.
Conservative treatment of osteochondrosis
Conservative treatment of osteochondrosis aims to relieve pain, normalize the function of the spine and its components, and prevent further degenerative changes in the human "axis".
Conservative treatment of osteochondrosis includes:
Drug therapy.It is used to relieve pain and inflammation of the tissues that make up the spine, as well as normalize metabolic processes.
To relieve pain and inflammation, various therapeutic restrictions are also used.Moreover, they help reduce muscle-tonic syndrome.Among therapeutic restrictions there are: trigger point restrictions, as well as intraosseous, facet, paravertebral and epidural restrictions.
Physiotherapy.It is used to relieve pain, increase the effectiveness of drug therapy and during the recovery period.Treatment is carried out using ultrasound, laser, magnetic field, low frequency current, etc.
Physical therapy (physical therapy), kinesitherapy.Specially selected dosed exercises are aimed at correcting the muscle corset, strengthening it, correcting posture, normalizing the function of muscle tissue and its flexibility, decompressing nerve roots, and preventing possible disease complications.All of the above is achieved by normalizing the metabolism and nutrition of the intervertebral disc, blood circulation, restoring the distance between the disc and the vertebrae, and distributing the load on the entire musculoskeletal system.
massageUsed to improve blood circulation, relieve spasms and tension in muscle tissue, and improve overall health.
Hydromassage.Helps to normalize blood circulation, metabolism, increase the tone of muscle tissue, and normalize the function of the nervous system.It involves massaging the body using a targeted stream of water with a certain pressure.True, in recent years, hydromassage has been adopted with the help of air bubbles applied to the body in a specially equipped bath or pool.
Manual therapy.It is used according to an individually selected program, targeting the musculoskeletal system.Helps improve blood and lymph circulation, metabolism, mobility of the musculoskeletal system, strengthens the immune system and prevents possible complications.
Extension (traction) of the spine.It is used with the help of special equipment to increase the intervertebral space and correct the structure of the spine, which usually leads to a reduction or complete removal of pain.
The use of a combination of the above methods to treat osteochondrosis has a good effect.
Medicines for osteochondrosis
Among the drugs for osteochondrosis are:
- Anti-inflammatory drugs.
- Antispasmodic.
- Antioxidants:vitamin C, vitamin E.
- Stimulator of blood microcirculation.
- Meant to prevent further degeneration of cartilage tissue.
Diet for osteochondrosis
For osteochondrosis, you need to eat 6 times a day, in small portions, drink at least 1.5 liters of water every day.
What can you eat with osteochondrosis:dairy products, lean meats (chicken, beef), jelly, jelly fish, jelly meat, fresh vegetables (tomatoes, cucumbers, onions, carrots, beets, peppers, cabbage, celery, broccoli), fruits, avocados, nuts, sunflower seeds, spinach, mushrooms, grains.
What should be minimized in the diet for osteochondrosis:grapes, legumes (peas, beans, etc.), flour products, hot seasonings, sugar, salty foods, meat soups and smoked meats.
It is better to steam food, because... With this method of preparation, the product retains the maximum amount of vitamins and microelements.
Try seasoning the salad with olive oil.
Surgical treatment of osteochondrosis
Surgical treatment of osteochondrosis is used when conservative methods are ineffective.Determined by the attending physician or physician council.It can also be used for severe damage to the spine and its components.
Treatment of osteochondrosis with folk remedies
Important!Before treating osteochondrosis at home with folk remedies, be sure to consult your doctor!
Treatment of osteochondrosis with ready-made herbal preparations
Comment by herbalist A.A.Malgin: herbal treatment (herbal medicine) has certain advantages, for example:
- herbal medicine eliminates the cause of disease,
- herbs have a minimal number of contraindications (usually individual intolerance),
- herbal treatments have minimal side effects,
- herbs contain a large number of vitamins and other useful substances, which, in addition to treating diseases, also contribute to the health of the body as a whole,
- affordable.
Herbalists offer ready-made solutions that have taken into account the specific composition of the collection, dosage, sequence, etc.These courses are developed by medical experts based on their years of experience.
Other folk remedies against osteochondrosis
dough.Prepare some dough from rye flour, 300 grams, and let it sit at room temperature for a few days.Drink a glass of milk and rub your back with turpentine.Then wrap the dough with gauze and apply it to the sore spot.Wrap with cellophane on top, and then with a scarf or towel.After a while, you may feel a burning and tingling sensation in the area, but bear it as long as you can.Do the procedure every day.Use each batch of dough no more than 3 times.
Sabelnik.Make a tincture of cinquefoil.Before going to bed, rub the area where your back hurts with the prepared tincture and tie a scarf around it.In addition, you can take a few drops of cinquefoil tincture before going to bed.
Ointment for osteochondrosis.Add 1 tablespoon to the container.a spoon of flour, 1 egg, 100 g of butter and 1 tbsp.a spoonful of vinegar, mix everything thoroughly and put it in a dark place for 2 days to infuse.Then remove any foam that has formed from the mixture.Mix the mixture well again and rub the resulting ointment on the sore spot.
turnip.Mix 300 ml of radish juice, 200 g of honey and 100 ml of vodka.Rub the resulting mixture on your back.This folk remedy also helps with radiculitis and rheumatism.
Prevention of osteochondrosis
To avoid pathological changes in the spine, follow these recommendations:
- lead an active lifestyle - swimming, running, doing morning exercises, riding a bike;
- pay attention to your posture during sedentary work - keep your back straight and keep your shoulders relaxed;
- perform sedentary work only on a comfortable chair, an armchair that can provide support to the spine;
- when working inactively, periodically exercise and warm up;
- sleep on a comfortable (orthopedic) mattress, pillow;
- try to avoid carrying heavy objects, and if you do, lift them slowly;
- do exercises to maintain excellent condition and pump your abdominal muscles;
- wear comfortable shoes, avoid wearing heels, especially during pregnancy;
- try to eat foods enriched with vitamins and microelements.
Which doctor should I consult for osteochondrosis?
- Vertebrologist;
- Neurologist;
- Osteopaths;
- Orthopedic Specialist.



















